Breast Enlargement
Breast Augmentation
Cosmetic breast enlargement using the surgical insertion of artifical implants is an option for women who are not satisfied with their existing breast shape or size. This may be due to insufficient development of breast tissue to their liking, from disease or trauma, or post pregnancy and breastfeeding resulting in loss of tissue volume (atrophy).
The way you look projects a particular image to yourself, your partner, family, friends and colleagues. The way you feel about how you look can affect your self-esteem, which in turn affects your image and your confidence.
The most common reasons women choose to undergo breast augmentation are :
- To increase the volume of your existing breast tissue
- To correct or improve unequal breast size or shape
- To reconstruct breast following removal of breast tissue, e.g. after a mastectomy
Non surgical options to enlarge your breast appearance include using external prosthesis or padded bras. There are no exercises, hormones or other medication which can produce permanent enlargement of your breasts.
The decision to undergo surgery should always be your decision. It should only be made when you are satisfied that it is the right option for you, you feel well informed, your questions have been answered, and you feel comfortable with your care provider.
Please remember that your surgeon cannot guarantee that the surgery will correct all of your concerns, and predicting the exact size and shape of your breasts after surgery is not possible. The ongoing appearance of your breasts can be affected by hormonal factors, weight loss or gain, chest wall shape, and pregnancy or breastfeeding.
It is also important to understand that artificial breast implants generally do not last forever, and will eventually require replacement, which will involve further surgery.
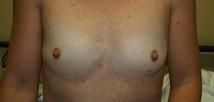
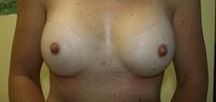
Patient Information
This information is not a substitute for a medical consultation.
The Implants ( Prosthesis)
Breast implants currently used in Australia consist of a silicone shell containing either silicone gel or a saline solution. There are numerous options available for cosmetic procedures, such as smooth or textured, round or tear shaped, and of course many different sizes. Different styles are used for different reasons, and the same implant could give different results in two different women. Sometimes two different sizes may be used to help equal the final breast size. Sometimes an additional procedure called a mastopexy ( breast lift ) may be recommended to achieve your desired result. It is important that time is taken to choose the right implant and the right procedure for you. Dr de Viana will discuss your options depending on your existing breast tissue, body weight and height, chest wall shape, and your desired result.
There is no medical evidence that breast implants cause cancer or other breast conditions, nor do they interfere with breastfeeding when the implant is placed appropriately. If you have concerns regarding your implants, please discuss them with Dr de Viana during your consultation.
The Position
Breast implants can be placed either in front of or behind your chest wall muscle. Generally, implants placed behind the chest wall muscle will give a smoother feel and appearance, and may reduce the risk of the implant rippling and / or hardening, and is the most common position for cosmetic breast enlargement. There are advantages and disadvantages for each position, and Dr de Viana will discuss those valid for you at your consultation, so you can make an informed decision of which position is best for you.
The Incision
There are 3 different incisions which may be used for implant placement :
- axillary ( armpit )
- periareolar ( around the nipple)
- inframammary fold ( the skin crease under your breast )
Each incision will be approximately 5 - 6 cm long, and will leave a scar. Although Dr de Viana will take due care to minimise scarring, occasionally scars become thick and red ( Keloid ). All scars take time to heal and fade. Dr de Viana will discuss the different reasons for choosing each incision and assist you to make a decision which best suits your body and your personal lifestyle requirements.
The Procedure
Breast enlargement surgery is performed by Dr de Viana under a general anaesthetic at an accrediated hospital, usually as day surgery. Patients may opt to stay overnight if it suits their personal needs, or Dr de Viana may recommend overnight stay if he feels it would be beneficial for your personal circumstances.
Dr de Viana will advise if any medical investigations or special requirements are necessary before your surgery.
It is important that you tell Dr de Viana if you have had any of the following :
- an allergy or bad reaction to antibiotics, anaesthetic, and or any medication
- any history of bleeding disorders or excessive bruising conditions
- any history of connective-tissue disorders such as rheumatoid arthritis, or lupus erythematosis , or other arthritic disorders
- any existing chronic illnesses or conditions or any recent acute illnesses
- any history of previous breast surgery or breast conditions, or previous radiotherapy to the breast
- any previous breast implant surgery
- any history of adverse scarring
- any history of psychological or psychiatric illness
- any current medications
- if you're a smoker
Smoking contributes to wound breakdown and delayed healing, as well as causing other health problems. Please be aware that any smoking immediately prior to or after your procedure may have adverse effects on healing and final cosmetic result.
Risks of Surgery
As with all surgery there are possible complications and you need to be aware of these to make an informed decision. Despite the highest standards of surgical practice, complications can occur.
- Anaesthesia - Modern anaesthesia is safe and effective, but does have risks. Rarely, these risks are life threatening. Any concern regarding your anaesthesia should be discussed with your Anaesthetist prior to your procedure.
- Wound infection- Although not common, this occurs in less than 10 % of cases and may require treatment such as antibiotics or local dressings. Most infections will be superficial ( in the skin ). Deeper infections are more serious, and can result in loss of the implant.
- Wound breakdown - This may occur due to poor or slow healing of the skin and breast tissue, or excessive stress on the wounds. Wound breakdown will significantly delay healing and may increase scarring.
- Bruising and swelling -This can take two to three days to develop, and may take a few weeks to fade. It may extend over your chest and abdomen or back.
- Bleeding (haematoma) - this may occur despite all care taken in surgery. Occasionally a second operation may be required to drain a blood clot.
- Scarring - There will be scars at your place of incision for each breast. Although efforts will be made to minimise scarring, scars can become raised and thick . While most scars fade and flatten over six months to a year, some may become "keloid" and remain raised, thick, itchy and red.
- Asymmetry- The shape and size can not be guaranteed between breasts. It is possible some difference will occur between size of breasts and positions of nipples. This is more common when asymmetry exists prior to surgery. A separate procedure may be necessary to correct marked asymmetry.
- Change of sensation in nipple and areola- More common with peri-areolar incisions, this is usually temporary, but sensation may take several months to return to normal. Occasionally this may be permanent. Additionally, nipple - areolar sensation may be increased.
- Loss of nipple and areola tissue - Very rarely, and again associated with peri-areolar incisions, the nipple and areola tissue can lose its blood supply resulting in complete or partial loss of the areola or nipple tissue. This would result in distortion and scarring at the site. Reconstruction by a skin graft may be possible to improve this.
- Allergic reaction - Occasionally, women may have allergic reactions to medical products such as suture material, tapes and lotions used during surgery. Reactions to the implants themselves are very rare.
- Breast feeding - Breast implants positioned behind the chest wall muscle should not interfere with breast feeding. However, existing breast tissue shape and volume may be altered by pregnancy and breast feeding, which may change the appearance of your breasts, even with implants in place.
- Heart and circulation problems - Although rare, a blood clot (thrombosis) can develop, usually in a leg vein. A clot can move to the lungs or heart where it can be life threatening. A chest infection is another possible risk after general anaesthetic. Early mobilisation/leg exercises should help reduce the risk.
After Surgery
Breast enlargement surgery is usually performed as day surgery. On discharge you need a friend or relative to drive you from the hospital, and stay with you overnight.
- Pain - During the first few days pain and discomfort are common, particularly when moving. Gradually pain should ease to become discomfort, which will typically fade in a week or two. Oral analgesics will be supplied and recommended to take when required as per Dr de Viana's advice. Excessive pain should be notified to our office.
- Drains - Although not used routinely, a plastic tube (drain) may be inserted into each breast to drain off any excess fluid if required. They remain in place until the drainage is minimal, usually only 1-2 days. Our nurse will remove the drains at our office.
- Bra - A surgical bra will be supplied . It should be worn at all times ( day and night) for 2 weeks. You should have a soft crop bra available for alternate wear when required during this time. As swelling caused by surgery subsides, size and shape of breasts will change. Individuals vary greatly in healing time, but soft tissue may take 3 months to settle. Appropriate support is important during this healing time. Underwire bras should not be worn in the first 6 weeks, or longer if there is delayed healing. Breast tissue will be affected by natural loss of support over time, and the wearing of supportive bras regularly will assist in minimising this loss.
- Sutures ( Stitches ) - Stitches are usually dissolvable. Any non-dissolvable sutures requiring removal will be attended by our nurse in Dr de Viana's office.
- Activity - It is very important to take things very easy for the first two weeks, but you should mobilize for short periods to improve circulation and to gradually increase activity. Getting out of bed after surgery and gently mobilizing will reduce the risk of postoperative complications including thrombosis (clots) and chest infections. Performing leg exercises, deep breathing and coughing exercises after surgery will also reduce your risk. Wear your TED (supportive) stockings whilst resting or sleeping for 2 weeks.
- Strenuous activities and heavy lifting must be avoided for 4 weeks. Strain on incision lines can lead to wound breakdown. Most women performing non-physical employment may return to work in approximately 7 - 10 days. If you perform physical employment, extended time off work may be necessary. You may return to gentle sporting activities after 6 weeks and should wear a supportive sports bra. Any complications following surgery would alter this advice.
- Driving - Do not drive until your range of movement and reflexes have returned to normal to allow for any sudden movements, usually 1 - 2 weeks. This can place strain on your incisions.
- Wound and dressings - Leave dressings in place until your first visit back at Dr de Viana's office. This is usually 3-5 days after your surgery. A small amount of visible ooze is normal, however excessive oozing (soaking the dressing) and leaking should be reported to our office.
Any redness around the wound or dressing, any unmanageable pain, or any fevers ( temperatures greater than 38 degrees ) should also be reported to our office.
Breast lumps may be noticed a few weeks after surgery, these are most likely due to small collections of fluid or blood. These should also be reported to Dr de Viana.
Implant Risks
- Capsular Contracture - Your body will form a capsule of scar tissue around your implant. This is a normal reaction to a artificial prosthesis. This tissue can thicken and harden, which in turn make your breast hard and painful. This condition can occur any time after surgery, sometimes in the immediate months following insertion, and sometimes many years later. If this contracture becomes severe, implant removal or replacement may be necessary.
- Fluid Collection - It is normal for some fluid to collect around the implant following insertion, causing swelling and discomfort. This can also happen after vigorous exercise or injury. If the collection is excessive, surgical drainage and / or other treatment may be necessary.
- Leakage or rupture of implants - This can occur due to injury, breast surgery, or very rarely, during radiological imaging to your breast. It is important to let your surgeon or Radiologist know you have implants in place. If an implant breaks or leaks, it cannot be repaired, and removal will become necessary. If your implant is saline filled, the saline is absorbed by your body ( and the implant will be deflated ). Modern silicone implants are made of cohesive gel, which minimises circulation of the gel content in the incidence of implant rupture.
- Implant movement - Implants may move from their original insertion position, and can cause changes in breast shape and / or breast discomfort. Surgery may be required to restore a desirable position.
- Implant extrusion - This is a rare occurence where the implant extrudes through the skin following severe wound breakdown, infection or radiotherapy. Implant removal would be necessary.
- Skin rippling - Most implants will develop some wrinkling over time, but do not alter breast feel or appearance. However, if the wrinkles are large, or breast tissue is particularly thin, ripples on the breast may be felt and seen.
Scar Management
Surgical tapes (eg Hypafix or Omnifix) can be applied to flatten scars and reduce stretching of suture lines. The tape can stay on for up to 7 days and it is recommended to continue with the taping for 6 weeks. Remove the tape if you feel that you are experiencing an allergic reaction or excessive irritation to the tape.
Scars will take 6-12 months to fade and for this period of time they may remain red and raised. After 6 weeks you can help flatten out scars by massaging the incision lines with moisturising cream daily.
After Hours Care
If you have medical concerns outside of our office hours, please attend Pindara Accident and Emergency Department, or your nearest emergency medical facility.
Final Result
Whilst Dr de Viana will make every effort to make your breasts look equal and to your desired appearance, and take every precaution to reduce the risk of complications, no guarantee can be given of the final cosmetic result. Differences in shape, size and symmetry may remain, and / or complications may occur. It is important that you take the time to read all the information supplied, and ask all the questions you have, and understand a realistic expectation of what can be achieved with cosmetic surgery.
Once you have decided to have surgery, it will be necessary for you to sign a consent form. You should not sign this form if you have unanswered questions or feel unsure of your decision. If for any reason you feel unsure about the advice being given, ask further questions, or seek an alternative opinion.





