Axillary Surgery
Sentinel Node Biopsy
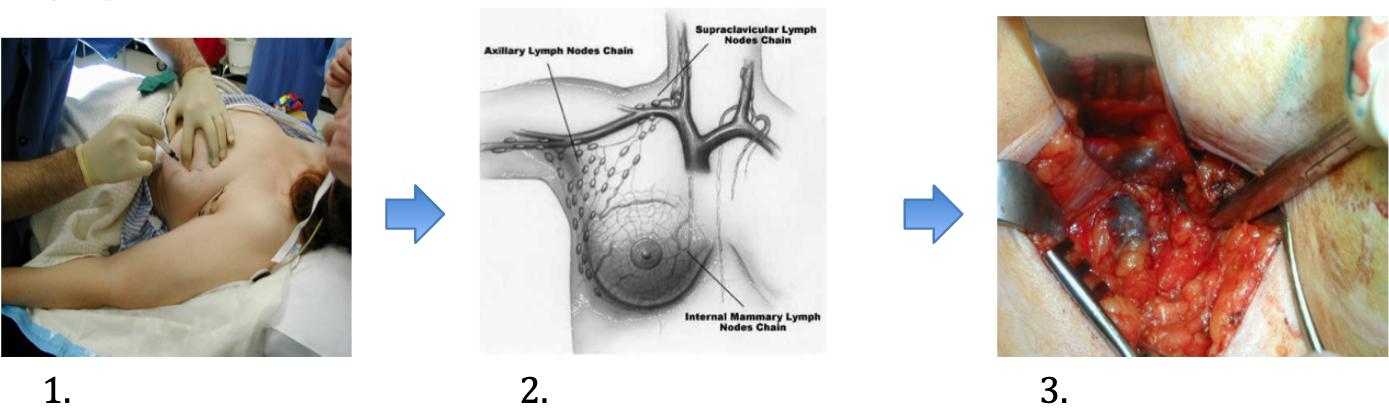
Sentinel lymph node biopsy is performed to assess whether there is any spread of breast cancer into the axilla. The technique is usually performed in conjunction with lumpectomy or mastectomy. Prior to surgery, an injection of dye (a radioactive isotope) is performed in the X-Ray Department. The dye is injected around the tumour and/or under the nipple. This dye is taken up into the lymphatic system and allows mapping of the lymphatic drainage of the breast. This is usually into the lymph nodes under the armpit (axilla) but may occasionally be toward the midline, between the ribs. It may take up to three hours to map which lymph nodes drain from the tumour site. The skin is usually marked over the lymph nodes of interest. During the surgical procedure, blue dye is also injected around the tumour to map out the lymphatic drainage in a similar fashion. At operation, an incision is made over the lymph node, which would most often be in the axilla. A small transverse incision , approximately 3 to 5 cm long, would be made in the axilla. A Gamma Probe allows identification of the lymph nodes containing dye. These are removed, usually 1 to 4 in number, and are sent for pathological assessment. The skin is closed with dissolvable sutures, and a drain is not usually required. Patients having lumpectomy and sentinel node biopsy can usually be discharged from hospital the day after surgery. Sentinel node biopsy reduces the risk of complications seen with a full axillary clearance, such as numbness, lymphoedema, and shoulder movement restriction.
Axillary Clearance
Removal of all of the lymph nodes under the arm is performed if there is moderate to heavy involvement of malignant cells in a lymph glands, either demonstrated on a prior sentinel lymph node biopsy or on needle biopsy of an abnormal lymph node pre-operatively. The treatment recommendations are constantly changing and currently if 1 or 2 lymph nodes are involved then sentinel node biopsy (see above) combined with axillary radiotherapy is as effective as an axillary clearance with potentially less risk of arm swelling (lymphoedema).
The majority of lymph glands under the arm draining from the breast region are removed. This number is variable but on average, between 10-30 lymph nodes would be removed. This may result in some numbness of the axilla and inner aspect of the upper arm. Physiotherapy is required to return range of movement in the shoulder back to normal. A small number of cases may develop swelling of the arm and/or forearm (lymphoedema). This risk can be minimised with regular physiotherapy and avoidance of infections in that arm. A drain is usually placed which may remain for a few days up to a few weeks , depending on the amount of drainage of fluid (seroma) from the surgical site. Drains can be easily managed at home. Even after removal of the drain, fluid may collect at the surgical site in the ensuing weeks, resulting in some swelling requiring painless manual drainage (performed at our office) with a needle and syringe (aspiration).





